Published on 31 October 2022
A look at treatments and therapy for communication impairment.

Ms Charilyn Ong from National University Hospital (NUH) became a Speech Therapist after her grandfather progressively became less communicative due to stroke and dementia. Witnessing the positive impact of speech therapy strengthened her desire to be part of this rewarding profession. She also finds it extremely rewarding to see the lives of her patients improve.
Today, she is seeing one of the clinic's long term patients, Mr Qusyairi. He was diagnosed with a rare leukaemia when he was 20 years old, and underwent an urgent craniectomy to remove the pooling of blood in his brain. This resulted in multiple communication impairments that limited his ability to communicate with his family and peers.

With intensive rehabilitation, he gradually made progress, and can now say simple greetings and short phrases. Given the severity of his impairments, however, he was introduced to Augmentative and Alternative Communication (AAC) in 2019. Today, Mr Qusyairi uses a 'Touch Chat' AAC application on his phone to construct phrases, before reading it aloud for him.
When compared to traditional AAC aids like picture cards, solutions such as apps allow the formulation of more complex ideas with increased vocabulary and grammar options. Ms Ong trains patients to use such apps as an avenue and alternative to express their needs and wants.

Aphasia is one of the communication disorders that makes it difficult for Mr Qusyairi to understand language, retrieve words and construct coherent phrases or sentences. It also makes it hard for him to coordinate motor movements needed to pronounce words clearly and accurately.
Such cognitive-communication deficits also impact his ability to express his emotions and interact with his peers. Here, Ms Ong is helping him construct functional phrases and sentences that he uses in his daily activities, such as ordering at a food stall, or recounting what he did over the weekend to his peers.

Therapy continues beyond the clinics as Mr Qusyairi’s family can also help him prepare short functional phrases and sentences which will then be used in his therapy sessions. During the session, Ms Ong reviews and edits them to increase his word bank, as well as work on Mr Qusyairi's sentence structure to help him improve his understanding and communication with others.
“If he encounters difficulty expanding his vocabulary or spelling new words, I will help him to input them by typing and selecting a corresponding picture,” said Ms Ong. “AAC is customisable according to the needs and preferences of the user. This is a rigorous process and Mr Qusyairi has been working with us for the past three years to expand his word bank.”

Not only do Speech Therapists work with patients to improve or regain their speech and language abilities, they also work to help patients gain independence and return to work or the community. After years of therapy in NUH, Mr Qusyairi has become more independent. With the support of Society for the Physically Disabled, he has found employment at Watsons, and uses his ‘Touch Chat’ app and communication cards in his daily interactions.
“His confidence has grown over the years, as he is able to interact with his family and peers, and contribute to society,” Ms Ong quipped. “Given that talking is intuitive for most of us, we may not realise the impact that communication disorders can have on someone’s participation, well-being, and relationships with others.
“I feel privileged to be supporting and advocating for our patients and their families throughout their recovery journey.”
Inpatient speech therapy
If you think Pictionary is hard, try it without gesturing or drawing the clues. Some patients experience that on a daily basis when they are recovering in the hospital, as they are too weak to speak or move their hands to write. With the use of AAC devices, Speech Therapists aim to help patients alleviate their communication difficulties.
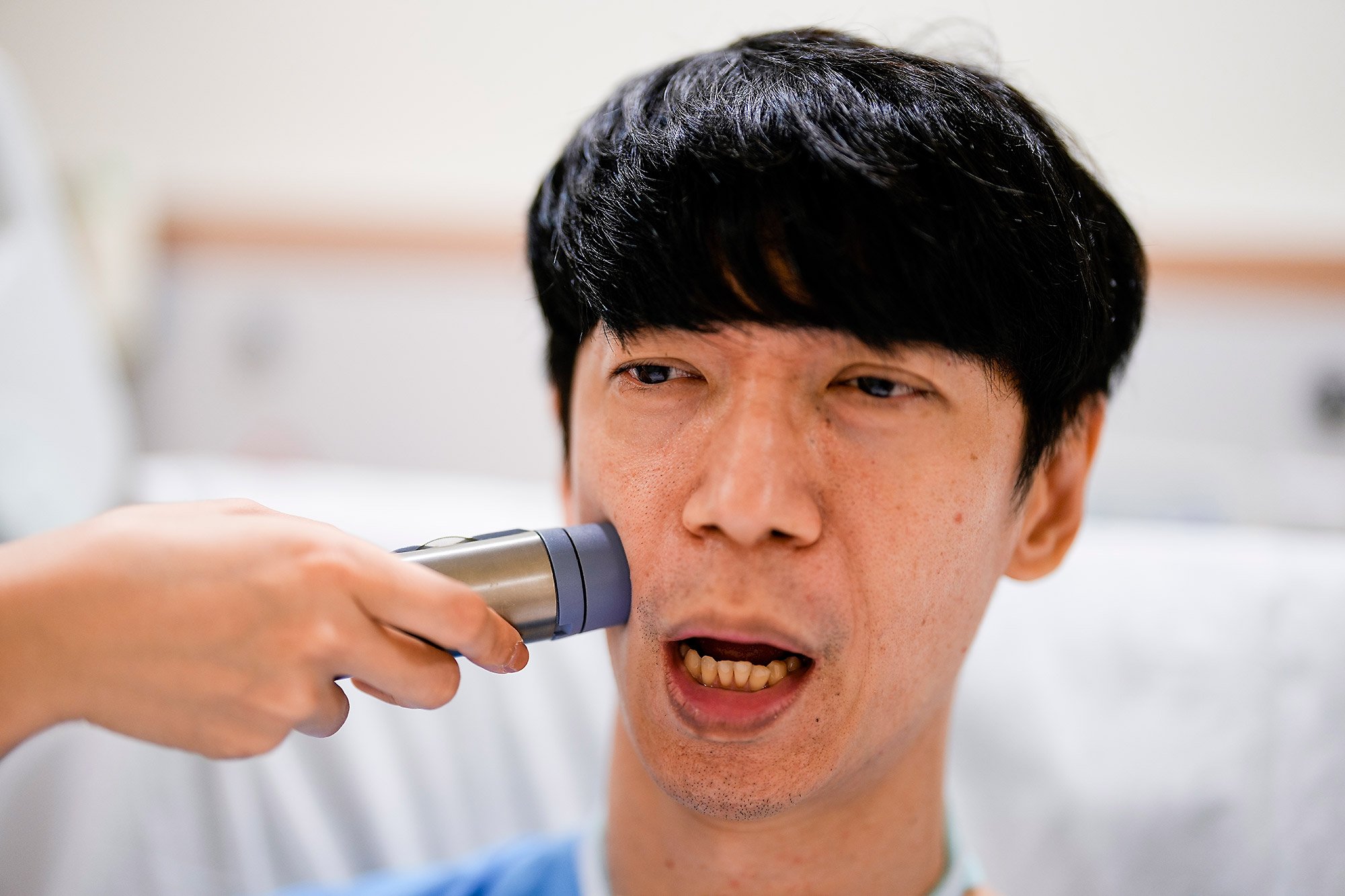
One such AAC is the electrolarynx. The device looks and sounds straight out of a sci-fi movie. It provides a tone which can be shaped by tongue, lips, palate or teeth, and translates it to a robotic and monotonous voice.

To use the electrolarynx, one places it on either the neck, face or in the mouth. Most of the time, patients with total laryngectomy (removal of voice box) after laryngeal cancer surgery will benefit from this device. As these patients lose their entire voice box, this device will substitute the voice box to produce a ‘voice’. Some patients were surprised that it sounds like a shaver at first, but with patience and practice, speech sounds will eventually become fairly intelligible.
Ms Poh Ailin from Ng Teng Fong General Hospital (NTFGH) teaches patients to find their best position for projection, and over articulate their mouth movements to enhance the clarity of the electronic voice.

For patients who are only able to move a certain part of the body, Ms Poh uses jelly bean switches connected to a tablet running AAC apps. When the buttons are pressed, it will make a selection on the app, allowing the patients to respond and make decisions.
“Even though we have not seen it before, we have read that it’s possible to use cheeks or even toes to press the switch!” said Ms Poh.

Choosing the type of AAC is dependent on several factors, including the patient’s language abilities and treatment goals. “Each patient has a different set of abilities for both receptive and expressive language skills. There is no one-size-fits-all approach. AAC needs to be tailored specifically for the patients.” explained Ms Poh.
How long patients need to use AAC devices also varies. Some patients use it for a short period to communicate while they recover. There are also instances where AAC devices become the primary mode of communication for the rest of their lives.

Eyes are the windows to the soul, and together with an Eye Transfer (E-TRAN) communication board, patients who have limited physical abilities and are unable to speak can actually ‘talk’ to Ms Poh.
At first glance, it looks like an acrylic board with stickers. But under the careful guidance of speech therapists, patients form words and phrases by using eye movement to spell it out letter by letter. It can be slow and tedious at the start, but with practice, this method can be efficient, and even fast, for some patients.
“Communication is a basic right, but it can be challenging for our patients. With various therapy techniques and devices, I hope to empower them with the ability to communicate again.” stressed Ms Poh.
Seeking help for your voice

Ms Jaymie Chai from Alexandra Hospital (AH) specialises in voice assessment and therapy at Alexandra Hospital. Most of her patients experience some sort of difficulty with their voices. Frequent voice users such as teachers, fitness trainers, and insurance agents form the bulk of patients seeking help.
“While most of my patients are between 25 to 50 years old, I see patients as young as 18 to the elderly in their 80s.” added Ms Chai. Sometimes, patients seek therapy because their voice does not match their age, like males who continue to have a high-pitched voice after puberty; it could also be patients whose voice does not match the gender they identify with.
Voice therapy starts off with education on how the voice is produced and the possible causes of a voice problem. Information on vocal health and acid reflux is essential for the maintenance of a healthy voice on a daily basis. The aim of voice therapy is to help the patient achieve a voicing technique that is least stressful or damaging to the voice box and sustainable for day-to-day use.

“You may need to see me if your sore throat doesn’t get better with Pei Pa Koa. So, please get it checked by an ENT (Ear, Nose, and Throat) specialist," said MsChai.
Benign growths such as vocal fold nodules or polyps, or excessive muscle tension when voicing, are common voice problems. In her clinic, she uses a voice analysis program to analyse her patient’s voice profiles. It creates visual representations of the voice in the form of spectrograms or waveforms, and provides numerical data on various aspects of the voice such as the pitch, loudness, and quality.

These programmes provide visual feedback and outcome measurements for patients to track their therapy progress. Most patients are usually keen to record their voice. “However, not all the acoustic data will be easily understood by them. Usually I’ll focus on the data that is the most meaningful and relevant to the patient, like pitch.” added Ms Chai.
A normal voice will have clear distinct bands in the spectrogram. A patient with a disordered voice that is creaky or breathy for example may have irregular or hazy-looking bands on the spectrogram.

One of the basic voice therapy techniques that Ms Chai teaches her patients in the clinic is voicing through a straw in water. To the untrained eye, it might seem like a tedious exercise of blowing bubbles in a cup. However, this simple step makes it easier for the vocal folds in your voice box to vibrate, effectively improving how your voice sounds.
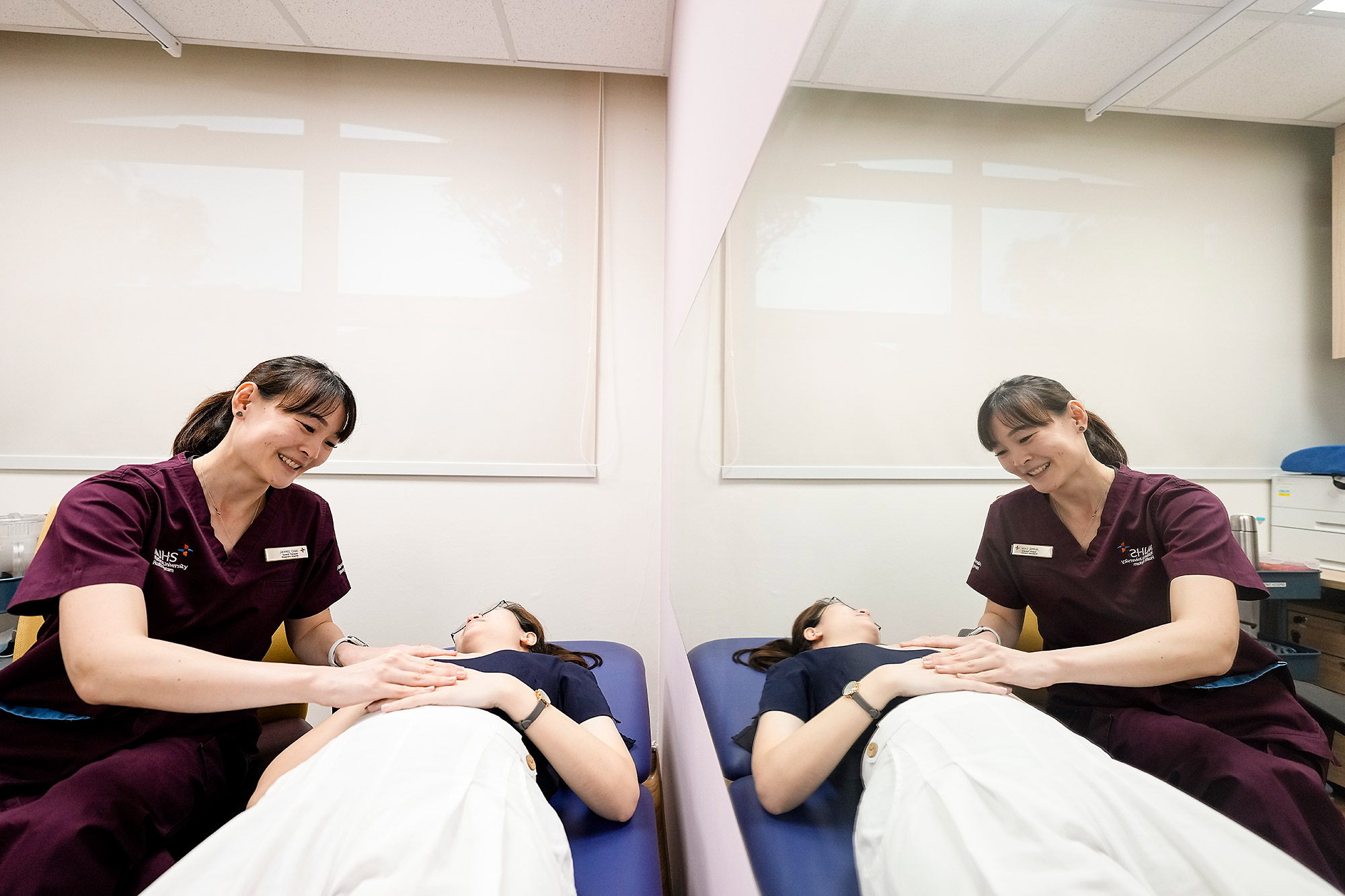
Do you sometimes get breathless when speaking? If that’s a yes, you might need to work on your diaphragm. Try this: breathe in through your nose and out through your mouth. When you breathe in, make sure your belly rises instead of your chest, and when you breathe out, your belly should flatten.
Diaphragmatic breathing is one of the exercises that Ms Chai does in her clinic. This exercise trains a stronger and more controlled diaphragm, which contributes to more effective voicing and also helps to manage symptoms of supragastric belching and acid reflux.
“Our voice is precious and forms a big part of communication and self-expression. To many of my patients, experiencing a voice change may feel as if a part of their personality has been taken away from them. On top of that, their daily struggle with maintaining their voice to keep conversations going at work or in their social lives takes a toll on their physical energy and mental health.” Ms Chai shared.
“I take joy in helping our patients achieve a healthier voice that is uniquely theirs.”
Click here to find out more or to join us as a speech therapist.
In consultation with Ms Jaymie Chai, Senior Speech Therapist, AH, Ms Poh Ailin, Senior Speech Therapist, NTFGH, Ms Charilyn Ong, Speech Therapist, NUH.




