Published on 10 March 2022
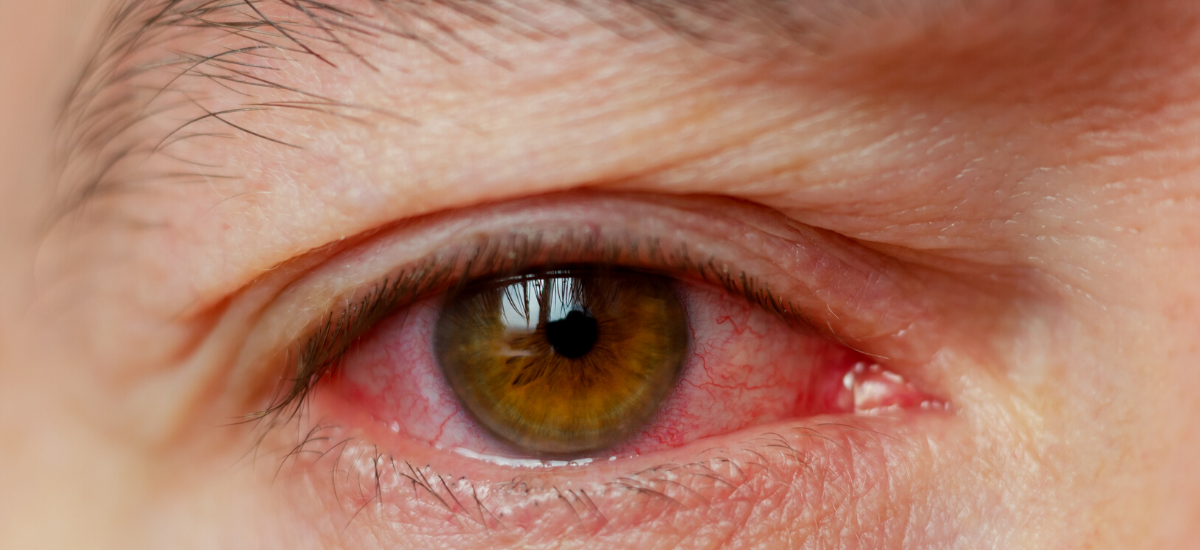
Do you frequently bump into things by accident? Have sudden eye pain, blurring of vision, headaches, nausea and vomiting? It might be glaucoma – a group of eye conditions that damage the eye nerve, an important structure that relays visual information from the eye to the brain.
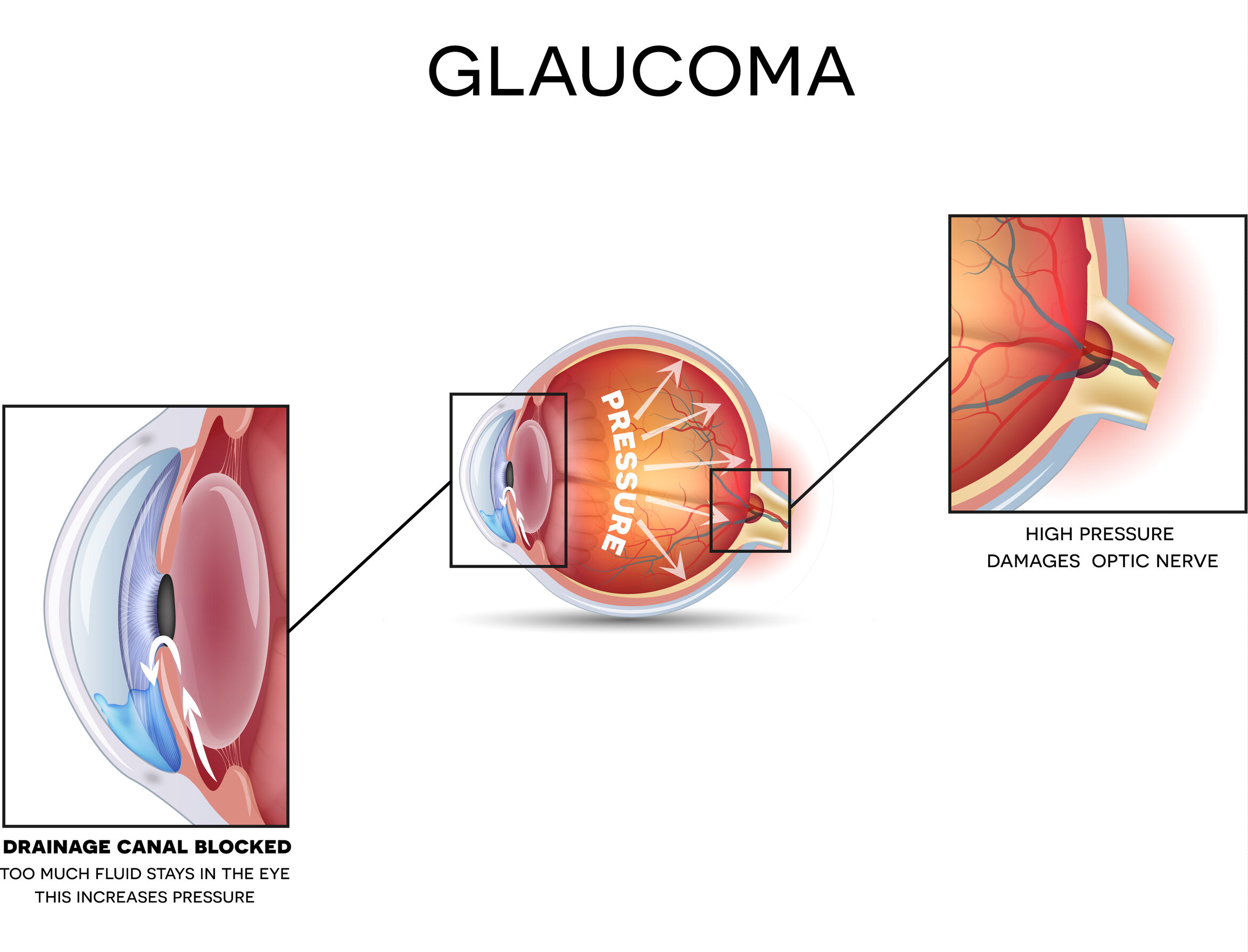
When a person has glaucoma, fluid in the eye builds up, leading to high pressure. Left untreated, this can eventually lead to permanent vision loss.
According to the World Health Organisation, glaucoma is the second leading cause of blindness in the world. And while it is true that glaucoma is more commonly seen in the elderly, it is a myth that glaucoma only affects them – in Singapore, 2-3% above the age of 40 suffer from glaucoma, a percentage that increases with age.
Glaucoma: the silent, incurable illness

At the initial stages of the disease, most glaucoma patients will experience a very gradual loss of vision, starting from the blurring of their peripheral vision. This may go unnoticed at first, but as the disease progresses over months and years, their central vision will start to blur as well.
And by the time patients realise they have the condition, it may already have progressed to quite an advanced stage.
“This is also why glaucoma is widely known as the ‘silent thief of vision’,” said Dr Katherine Lun, Consultant Ophthalmologist in the Department of Ophthalmology at the National University Hospital (NUH).
However, a small group of patients may experience more sudden symptoms. These include raised eye pressure including headaches, eye pain, seeing coloured rings (haloes) around lights, blurry vision, and nausea.
Such cases are considered eye emergencies and will require the immediate administration of medications to bring down the eye pressure, as well as a laser procedure to relieve fluid blockage, Dr Lun explained.
Managing glaucoma
Once diagnosed, doctors will attempt to lower pressure in the eyes to stall progression. The first line of treatment is usually a topical anti-glaucoma medication or laser treatment (laser trabeculoplasty).
If the patient is unable to tolerate the medications, or if progression continues despite treatment, surgery is offered. The three main categories of surgeries are filtration surgery (trabeculectomy), glaucoma drainage implants, and minimally invasive glaucoma surgery. These procedures aim to surgically reduce the eye pressure and slow down further damage to the eye nerve to help preserve vision.
While living with glaucoma can be challenging, it is highly treatable and manageable. “Even though we cannot cure glaucoma, it is important to remember that with appropriate treatment and compliance to therapy, most patients do well and maintain good vision for many years,” Dr Lun noted.
The most common challenge that Dr Lun has observed in her patients’ everyday lives involve the administration of eye drops. “This is especially the case with elderly patients who may experience difficulty with aiming and instilling drops. And if they have multiple eye drops, they may sometimes get confused with the type and frequency of drops,” she said.
Some patients also have difficulty moving around, she added. In such patients, their advanced glaucoma may cause symptoms such as a constricted field of vision and reduced contrast sensitivity. As such, they may have difficulty with stairs and an increased risk of falls, adversely affecting their quality of life.
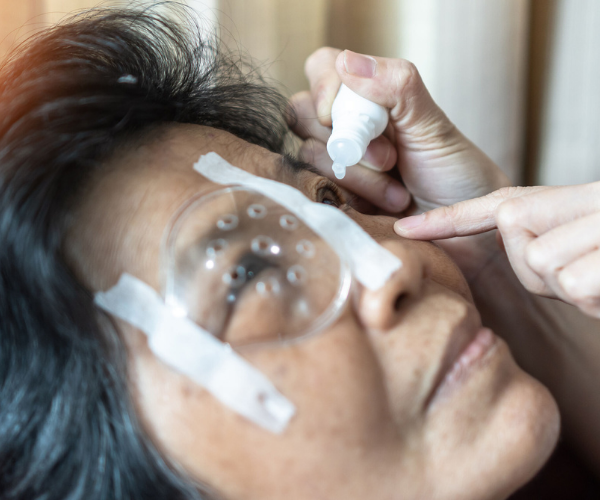
If you are helping to care for a loved one with glaucoma, especially an elderly loved one, you can help them manage and administer their eye drops: it is crucial that their medications are administered as prescribed and that they get regularly reviewed by their eye doctor.
And if patients face challenges moving around, arrange objects and furniture in the home so that they have clear paths and minimal obstructions to everyday tasks. They can also be referred to a Low Vision Specialist who may offer advice on how to cope with their condition.
“Vision loss due to glaucoma can impact patients in many ways - visually, functionally and psycho-socially,” shared Mr Daniel Bohan, a Senior Optometrist at NUH who runs the hospital’s Low Vision Service.
“A comprehensive low vision assessment and rehabilitation is helpful to help patients regain independence and improve their quality of life.”
Glaucoma and eye protection
Glaucoma patients may experience light sensitivity and glare on bright, sunny days, when driving, and sometimes even while working on computers.
Wearing sunglasses can help ease the discomfort when heading outdoors. Choose darkened, polarised lenses to block the glare.
When working on your computer, some tips to reduce glare issues include positioning your computer away from the window and avoiding overhead lighting. You can also consider fitting a good filter over your screen to reduce the glare.
Early detection and treatment

Prevention is always better than cure. If diagnosed and treated early, blindness from glaucoma is potentially preventable, said Dr Lun.
Since glaucoma is hard to notice, afflicted individuals may not even realise they are experiencing visual field loss until it is too late. As such, regular eye screenings can help detect disease early – and with at-risk individuals, such as those above the age of 40, with a family history of glaucoma, or who are on long-term steroid medications, more frequent eye screenings may also be required.
“Being diagnosed with glaucoma is not a death sentence to vision,” concluded Dr Lun. “With early diagnosis and good control of eye pressure, many patients can still lead fulfilling and active lives.”
“It is thus important to go for regular eye screens to allow the early detection of the condition.”
In consultation with Dr Katherine Lun, Consultant, Department of Ophthalmology, NUH; and Mr Danial Bohan, Senior Optometrist, NUH.