Published on 19 January 2023
Thyroid cancers are one of the most common head and neck cancers in the world, with the past decade seeing a significant increase in their incidence.
Thyroid cancer is more common in women than in men. In Singapore, it is the eighth most common cancer diagnosed in women and is also commonly diagnosed in younger patients: most patients are below 60.
”With advances in imaging capabilities, identification of thyroid cancers before patients develop symptoms is not uncommon and early detection always means more effective treatment options,” Dr Donovan Eu, Consultant at the Department of Otolaryngology, National University Hospital (NUH) and Division of Surgical Oncology, National University Cancer Institute, Singapore (NCIS) shared.
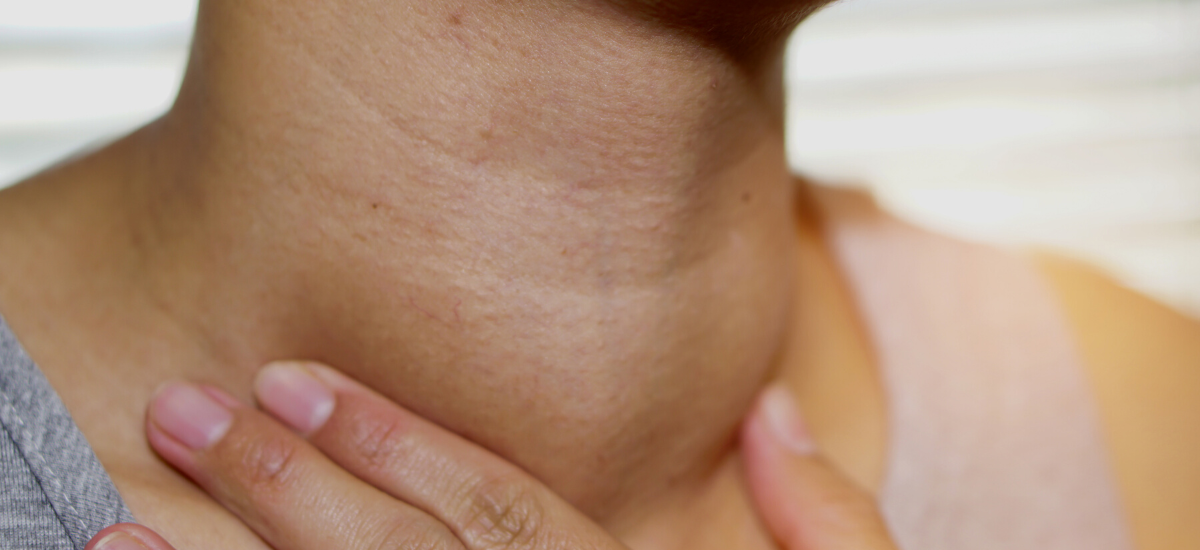
Thyroid cancer affects the thyroid gland – a small, butterfly-shaped gland at the base of the neck that produces hormones. Dr Eu noted that this class of cancer is broadly divided into two groups: differentiated thyroid cancers – of which papillary thyroid cancers account for the vast majority of cases seen worldwide – and anaplastic thyroid cancers. Anaplastic thyroid cancers often have a poorer prognosis but are fortunately less common.
The main symptom of thyroid cancer to look out for is a painless, slow-growing lump or mass at the centre of the neck. Lumps can also occur at the sides of the neck in cases where cancer involves the surrounding lymph nodes.
“In advanced cases, some patients may develop changes to their voice, difficulties swallowing and/or breathing, or coughing up blood. Thankfully, the presentation of these symptoms is less common,” Dr Eu further explained.
If your doctor suspects that you have thyroid cancer, he or she will carefully examine your neck, lymph nodes and sometimes voice box to determine the extent of the disease. An ultrasound may be ordered to further evaluate the lump and look for sonographic features that may help with diagnosis.
In some patients, a needle biopsy is performed to look for cancer features under a microscope. Dr Eu noted that the needle biopsy is reliable, with a relatively high rate of accuracy in thyroid cancer detection.
Surgery remains the current standard treatment
If confirmed, surgery to remove the thyroid gland remains the mainstay of treatment. Depending on the extent of involvement, this may involve the removal of half or even the entire thyroid gland. In addition, evaluation and possible removal of the regional lymph nodes may be performed in the same procedure. Skilled surgeons are necessary in order to avoid injury to the nerve of the voice box, which lies close to the thyroid gland. Your surgeon will also work to preserve the small parathyroid glands nearby that regulate the body’s calcium.
In general, patients can be up and about fairly quickly: most can resume eating, drinking, and talking almost immediately after surgery and some may need to rest at home for about one to two weeks before resuming normal activity. Those patients who have undergone surgical removal of the entire thyroid gland may require hospitalisation for a few days to monitor for calcium disturbances. All patients will require thyroid hormone replacements following removal of the entire thyroid gland and in some cases, a period of calcium supplements may also be required.
After surgery, the use of radioactive iodine may be needed as well, depending on pathology results. This is administered by nuclear medicine or radiation oncology doctors and may require a short second hospital stay. Such combined treatment achieves good outcomes for patients and Dr Eu stated that “90% of patients diagnosed with thyroid cancers are potentially cured”.
New advancements in treatment and management
The use of gene testing allows for greater accuracy and further refinement of a patient’s prognosis, Dr Eu said. “Information from gene testing can also be incorporated into treatment planning, thus personalising care for patients.”
More recently, there has also been a shift in thinking in the management of early-stage thyroid cancers. Dr Eu explained, “There are studies demonstrating that low-risk thyroid cancers may remain dormant even after more than ten years. In closely monitored cases, small low-risk thyroid cancers have been observed with great success in ultrasound imaging to determine that the cancers in question are stable over a long period.”
“This body of evidence has helped us to understand more about the disease, thereby avoiding unnecessary surgeries and their inherent risks.”
Treatments in development
Several minimally invasive treatments are also currently being evaluated, including “endoscopic thyroid surgeries, robotic thyroid surgeries and radiofrequency ablation”, added Dr Eu. “The recent integration of technologies such as nerve monitoring has also allowed for safer surgeries in complex conditions, improving outcomes.”
For advanced thyroid cancers, several advances have also been made: novel targeted therapy is one. Such therapies use medications that attack specific features of cancer to stop its growth or spread. Tyrosine kinase inhibitors (TKIs) have been successfully used in the treatment of some cancers and represent another avenue in the treatment of complex conditions, leading to significant improvements in patients’ outcomes. While novel targeted therapies are still undergoing further clinical trials, early results have shown great promise.
Thyroid cancer is not a death sentence
With timely and appropriate treatment, thyroid cancers are certainly curable. Those who present with more advanced or complex thyroid cancers can also expect ongoing developments in diagnostics and treatment to further improve the care, treatment and management of their conditions. If you suspect that you have thyroid cancer, seek medical attention immediately. Early detection is key to beating this disease.
In consultation with Dr Donovan Eu, Consultant, Department of Otolaryngology-Head & Neck Surgery, NUH and Consultant, Division of Surgical Oncology, NCIS.