Published on 4 April 2022
Colorectal cancer patients with disease previously considered incurable may soon have an option for treatment, a study by NUHS clinicians has found.
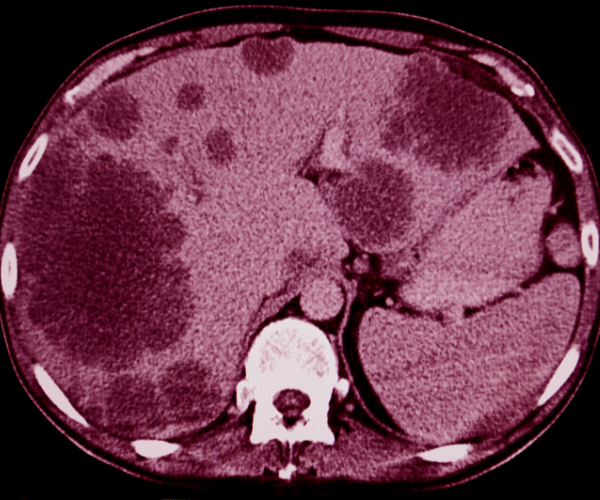
One of the most common cancers in the world, colorectal cancer has a tendency to spread (or metastasise) to the liver – a phenomenon that occurs in around 40 per cent of patients.
Liver metastasis is one of the biggest killers in colorectal cancer patients. The good news: if caught early enough, it can be treated effectively with a combination of surgery and chemotherapy.
But once the liver spread becomes too extensive, patients are considered inoperable, and are hence left without further options for cure – even if they are still physically fit and strong. In such circumstances, patients typically only have the option to undergo chemotherapy, in a bid to prolong their lives.
But “we should not just write off colon cancer patients with cancer that has spread to their livers,” said the study’s lead author, A/Prof Glenn Bonney.
In theory, a liver transplant could be a solution. However, such a procedure has long been seen as too risky an endeavour for these patients, potentially causing more harm than good.
“Traditionally, there was fear of transplanting such patients…their immune system has to be suppressed to enable the surgery, and as a result the cancer may come back very aggressively,” said A/Prof Bonney, Consultant at the Division of Hepatobiliary & Pancreatic Surgery at the National University Hospital (NUH).

But when done in a well-coordinated manner and in well-selected patients – liver transplants may in fact be a feasible treatment option, posits the study, which was published in September 2021 in scientific journal Lancet Gastroenterology and Hepatology.
Drawing on the knowledge gleaned from three decades of previous studies, the clinicians formulated a practical patient management algorithm that proposes a series of guidelines for treating these patients.
The guidelines take into consideration factors such as the biological behaviour of cancer in response to therapy, as well as the involvement of a multidisciplinary team of experts in the patient selection process, including pathologists, radiologists, surgeons, hepatologists, and oncologists.
Under these guidelines, between 5 and 10 additional patients a year in Singapore – who were previously deemed to have incurable disease – could now receive treatment.
“This strategy, in well-selected patients, offers a potential cure when selected and investigated well,” A/Prof Bonney noted.
Dr Mark Muthiah, another of the study’s authors who is Consultant at NUH’s Division of Gastroenterology and Hepatology, agreed that the biggest risk of a transplant in such patients is the chance of the cancer recurring afterwards.
“The clear algorithm determined by the consensus group helps doctors select patients who can avoid this,” he explained.
With the treatment set to be put into practice within NUH, the study’s authors have opened an international collaboration in living donor transplantation, in hopes of pooling their expertise, improving their understanding of the disease, and taking their work one step further.
“In Asia, including at NUH, we have worldwide published excellent results in living donor liver transplantation,” said A/Prof Bonney, adding that a number of Asian centres with expertise in cancer and transplantation have expressed keenness to participate.
“Therefore, we are in a good ecosystem to be able to perform this, and add to treatment options of these patients.”
In consultation with A/Prof Glenn Bonney, Consultant, Division of Hepatobiliary & Pancreatic Surgery, Department of Surgery, NUH; Consultant, Liver Transplantation, NUCOT, NUH and Consultant, Division of Surgical Oncology, NCIS and Dr Mark Muthiah, Consultant, Division of Gastroenterology and Hepatology, Department of Medicine, NUH and Consultant, Liver Transplantation, NUCOT, NUH.