Published on 18 March 2026
Doctors at NUH are studying whether artificial intelligence can help detect stomach cancer at an earlier, more treatable stage.
At a glance
- Stomach cancer is often diagnosed late because early symptoms are not obvious during routine examinations.
- A new AI system is being tested to help doctors spot subtle warning signs during endoscopy.
- Early results suggest AI can support doctors, especially in identifying precancerous changes that are easy to miss.
Stomach cancer often develops quietly. By the time symptoms appear, the disease may already be advanced, making it harder to treat successfully.
As a result, it remains one of Singapore’s deadliest cancers, with around 300 to 500 lives lost each year.
A key challenge is that many cases are detected only at a later stage.
“Put simply, early detection improves survival,” said Dr Daryl Chia, Consultant, National University Centre for Digestive Health (NUCD), National University Hospital (NUH). “As stomach cancer becomes more advanced, the chances of survival decrease.”
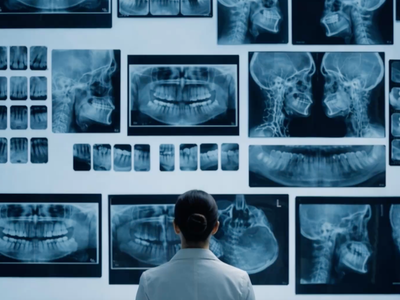
Diagnosis usually begins with an endoscopy, a procedure in which a thin, flexible tube with a camera is passed into the stomach. This allows doctors to examine the stomach lining closely and take small tissue samples from suspicious areas.
However, in the early stages, these abnormal areas may appear flat and subtle, and can also be obscured by inflammation in the stomach lining. As a result, early signs of stomach cancer can be easily overlooked, and many patients are diagnosed only when the disease is more advanced.
Where technology can make a difference
To address this gap, Dr Chia and his team conducted a study to find out whether artificial intelligence (AI) could help improve the early detection of stomach cancer.
They worked with a Japanese company founded by a gastroenterologist and endoscopist to develop an AI platform that could identify early and subtle abnormalities in the stomach lining.
The AI system was trained using thousands of endoscopy images and videos, so that it could learn to recognise patterns associated with cancer and precancerous changes. Once its accuracy was assessed, doctors in Singapore began testing its performance in local clinical practice about three years ago.
During these tests, the AI reviewed endoscopy images and highlighted areas it considered suspicious. These findings were then compared with the assessments of experienced specialists.
Overall, the AI performed at a level similar to that of doctors. Notably, it was better at identifying high-grade dysplasia, a serious precancerous condition that can be particularly easy to miss.
“That was an encouraging sign for us,” said Dr Chia.
Testing in real time
The next step was to test the system during live endoscopy procedures, where Dr Chia believes it could offer the greatest benefit.
“The goal is not for AI to replace doctors, but to act as a second pair of eyes during real-time endoscopy,” Dr Chia explained. “It adds an extra layer of checking.”
Specialised equipment was installed in the endoscopy suite so that the AI system could analyse the live video feed. During each procedure, it would highlight areas of concern and generate a score from zero to 100 to indicate how likely a particular area was to be cancerous.
Dr Chia clarified that the score itself is not a diagnosis. Instead, it serves as a guide to draw the doctor’s attention to areas that may warrant a closer look or a biopsy.
“The number is not absolute,” Dr Chia said. “What matters is how we interpret it in the context of the patient and what we see during the procedure.”
The study also found that procedures assisted by AI took slightly longer, which Dr Chia noted was expected.
“There is a learning curve, and we are mindful of how AI affects workflow as we move forward,” he said.
For now, the findings suggest that AI’s role in detecting stomach cancer is supportive and strengthens rather than replaces clinical judgement.
Dr Chia said: “If it helps us catch cancers earlier, reduces unnecessary biopsies and supports doctors at different levels of experience, then it has real clinical value.”
|
Other ways AI is used at NUH Artificial intelligence is already embedded in everyday practice at NUH, supporting both clinical care and hospital operations. • Pathfinder (Emergency Department) Uses real-time data to track waiting times, bed occupancy and patient flow in the Emergency Department. By predicting daily patient turnout, it helps teams deploy manpower more effectively and reduce bottlenecks. • CalSense+ (early disease detection) Automatically flags abnormal calcium levels in blood tests, enabling earlier detection and treatment of hypercalcaemia. This reduces delays in care and supports faster clinical decision-making across NUH and partner institutions. • Russell-GPT (clinical workflow support) Assists doctors with administrative tasks such as summarising case notes and drafting referral letters. By reducing paperwork, it allows clinicians to spend more time on direct patient care. |
In consultation with Dr Daryl Chia, Consultant, NUCD, NUH.