Published on 17 August 2023
It’s common to seek out acupuncture to treat your aches and pains. But did you know that acupuncture can be used to treat other conditions as well – such as in stroke rehabilitation?
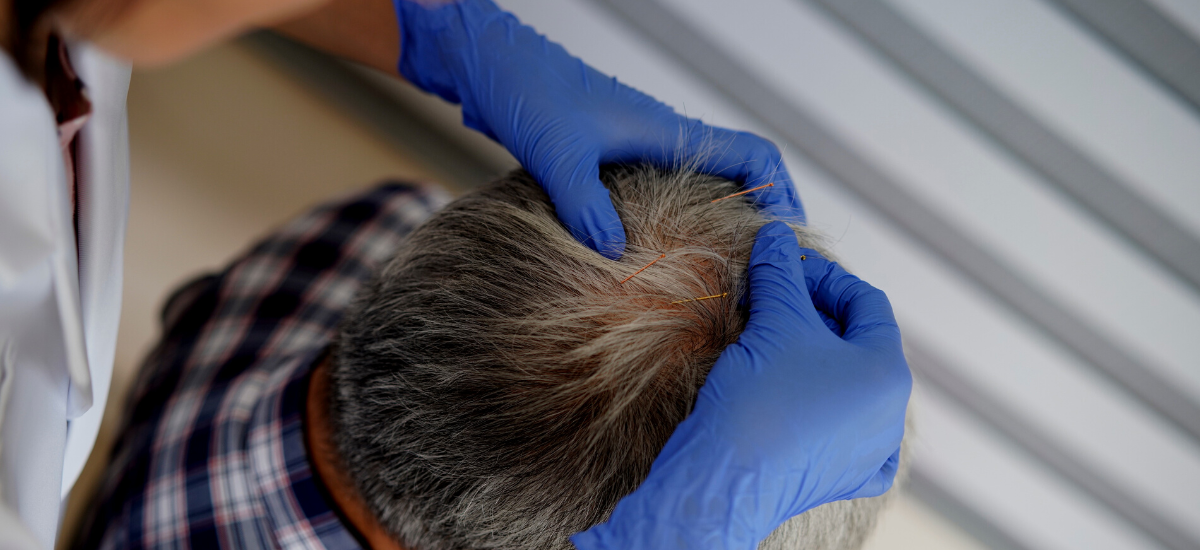
Most Singaporeans would be familiar with the ancient Chinese practice of acupuncture. Dating back as far as the Chinese Stone Age, the therapy involves using very thin, solid needles to stimulate anatomical points on the body. This, according to the principles of traditional Chinese medicine (TCM), helps to balance a person’s life force, or qi.
Today, acupuncture is a well evidenced form of alternative pain management, with many turning to the therapy as a safe, medication-free way to treat pain conditions from muscle strains to migraines.
But what is lesser known is that acupuncture can also be used in other areas of treatment – including stroke rehabilitation. Senior acupuncturist Dr Qiao Tian Ru from the National University Hospital (NUH) shares more.
Acupuncture in stroke rehabilitation
In most hospitals in the Western world, stroke rehabilitation is carried out by a team of doctors, nurses, and allied health practitioners like physiotherapists, occupational therapists, psychotherapists, and speech therapists.
Such a multi-pronged approach is necessary because depending on the region and the type of stroke, effects can vary widely: from sensorimotor problems like paralysis, to cognitive and emotional problems like depression, anxiety, and memory loss.
But in Chinese hospitals, there’s one additional, indispensable member of the rehab team – the acupuncturist.
“Stroke is a very complex disease affecting different locations of the brain,” Dr Qiao explained. She added that strokes can fall under two main categories, haemorrhage strokes and ischemic strokes. Around 80% of strokes are ischemic, which means they’re caused by blockages in the blood vessels.
“In such cases, the supply of blood to the brain tissue is blocked, causing cell damage or death,” she said. Depending on the location of the injury within the brain, patients may experience symptoms like dizziness, speech impairment, partial or full paralysis, loss of balance or coordination, and sensory issues – in some cases numbness, in others excruciating pain.
And while acupuncture is certainly no silver bullet, evidence suggests that it may be effective in treating several of these symptoms. This, said Dr Qiao, works because the needles stimulate the brain and body to produce natural painkillers called endogenous opioids. These can help to control various aches and pains, such as shoulder pain, a common symptom among post-stroke patients.
It’s not just pain, either. Clinical trials have demonstrated the efficacy of acupuncture in improving balance function, reducing spasticity, and increasing muscle strength post-stroke. One trial in particular showed that electroacupuncture, when combined with exercise therapy, was more effective in improving limb function in stroke patients than exercise therapy alone – possibly because with less pain and more relaxation, patients are able to undergo their therapy more effectively.
One point to note is that acupuncture does not aim to treat individual symptoms, but the patient’s overall condition. “It’s a human, holistic treatment,” Dr Qiao said. “In acupuncture, we connect with people through touch, through anatomical points on the body.
“Of course, we do use specific points to treat different symptoms – their depression, their muscle spasms, their weakness – but what we aim to do is to treat the patient based on his or her overall condition.
“So this may cover a wide range of symptoms, such as paralysis, mood, appetite, bowel movement, pain, and even sleep quality.”
Working towards better evidence
While the effectiveness of acupuncture has been fairly easy to track, the precise mechanisms behind its beneficial effects remain unclear.
Much of the issue lies within the difficulty in translating TCM principles to Western medicine. “We explain our words in a different way in TCM,” said Dr Qiao. “Our concepts are not based on physical elements like tissues and cells; they’re based on things like yin and yang and qi. It’s completely different from modern, Western science.”
Furthermore, the manner in which trials are designed in the Western world are fundamentally at odds in the way in which acupuncture is carried out – a major obstacle to getting the therapy recognised as mainstream.
“On the clinical side, on the historical side, we’ve seen plenty of benefits. But it’s difficult to design a proper, beautiful, gold-standard study for acupuncture,” Dr Qiao said. The gold standard in Western medicine is a double-blind randomised controlled trial, in which a placebo is compared with the experimental treatment, with neither the participant nor the researcher knowing who received what.
Unfortunately, double-blinding isn’t possible in acupuncture, nor is placebo treatment – a challenge also faced by the surgical field. Unlike surgery, however, it’s far more difficult for an alternative therapy to obtain the resources needed for research.
Furthermore, acupuncture is also rarely used as a standalone treatment. A diagnosis in TCM often results in an individualised treatment plan, combined with other forms of therapy or herbal medicine. This makes its precise effects even harder to isolate, posing an even greater challenge to research.
And while more and more studies have been conducted in more recent years – “we still do not have enough evidence, by Western medicine standards,” said Dr Qiao.
“But lack of evidence of an effect, does not equal evidence of the lack of an effect.”
The long road
Having been with the acupuncture team at NUH since its inception in 1999, Dr Qiao has watched public perception of the therapy change over the years.
“In spite of its long history and widespread use, acupuncture was still considered a new therapy in mainstream hospitals. So initially it was very difficult here,” she said. “People don’t trust you…and that’s because unlike Western medicine, our roots are in patients’ satisfaction – not in clinical studies.”
In fact, at the start, the clinic was only able to offer half-day sessions. Back then, they would only get referrals from the orthopaedics department, to treat back and neck pain under combined regimens of physiotherapy and acupuncture. “Because you often can’t do very invasive treatment when it comes to the spine, especially for elderly patients,” Dr Qiao explained. “So this was a safer, more conservative way to treat chronic pain.”
At the time, acupuncture services were not subsidised by the government. Still, the clinic continued to grow – and just a year later in 2000, it became a full clinic. Referrals began to come from other departments as well.
“Even without subsidies, we survived,” she said. “Our patients gave positive feedback to their doctors…so although at first the doctors here didn’t know much about acupuncture, they later began to recommend referrals to our clinic.”
With increasing awareness, patients of all races have become more receptive to the therapy. This led to a milestone move in 2020 when the Ministry of Health announced a pilot programme to provide subsidised acupuncture treatment for lower back and neck pain at public specialist outpatient clinics.
Today, the clinic gets 12,000 visits a year and is staffed by three full-time acupuncturists. But Dr Qiao hopes that public understanding of acupuncture will continue to grow.
“Compared to Western medicine, acupuncture is still based on a different philosophy. So it’s still not accepted by everyone,” she conceded.
“But I believe TCM has a place in today’s society, as a natural, affordable, and holistic treatment. It’s not a silver bullet, but it does do certain things very well…and so I hope that we can study TCM’s effects on a greater number of conditions in future, and increase public acceptance of acupuncture as an active part of the health system to prevent and treat diseases.”
In consultation with Dr Qiao Tian Ru, Senior Acupuncturist, Department of Anaesthesia, NUH.