Published on 28 April 2026
An NUHS tele-dentistry programme is helping children at risk of caries receive earlier assessment, clearer guidance and faster follow-up care.
At a glance
HEADS-UPP tele-dentistry brings dental risk assessment into preschools serving lower-income families.
Personalised dental reports and tiered referrals are improving follow-through on treatment and preventive care.
Early findings suggest lower caries risk and stronger parental confidence after follow-up.
Dental disease in young children is often detected only after pain, visible decay, or feeding difficulties appear. By then, treatment can be more invasive, more distressing and harder for families to navigate.
A tele-dentistry programme under the National University Health System (NUHS) is seeking to move assessment earlier and bring clearer follow-up pathways closer to at-risk children.

A/Prof Catherine Hong (far left), Adj A/Prof Chong Shang Chee (second from right) and Dr Ishreen Dhillon (right) with families who had benefitted from the HEADS-UPP tele-dentistry programme.
Local data highlights the scale of this gap. Around 48 per cent of preschool children aged 1.5 to four in Singapore have dental caries, of which 90 per cent of affected children remain untreated. Among lower-income children advised to seek follow-up dental care, only 13.3 per cent did so within three to four months.
Moving dental assessment closer to families
The tele-dentistry programme sits within the HEAlth and Development Support in Preschool Partnerships (HEADS-UPP), a broader preventive health initiative delivered with preschool and social sector partners for children from lower-income families.
Dental assessment is brought into preschools, reducing reliance on symptom-led clinic visits and allowing risk to be identified earlier. Typically, parents complete a questionnaire adapted from the American Academy of Pediatric Dentistry’s caries risk assessment tool.
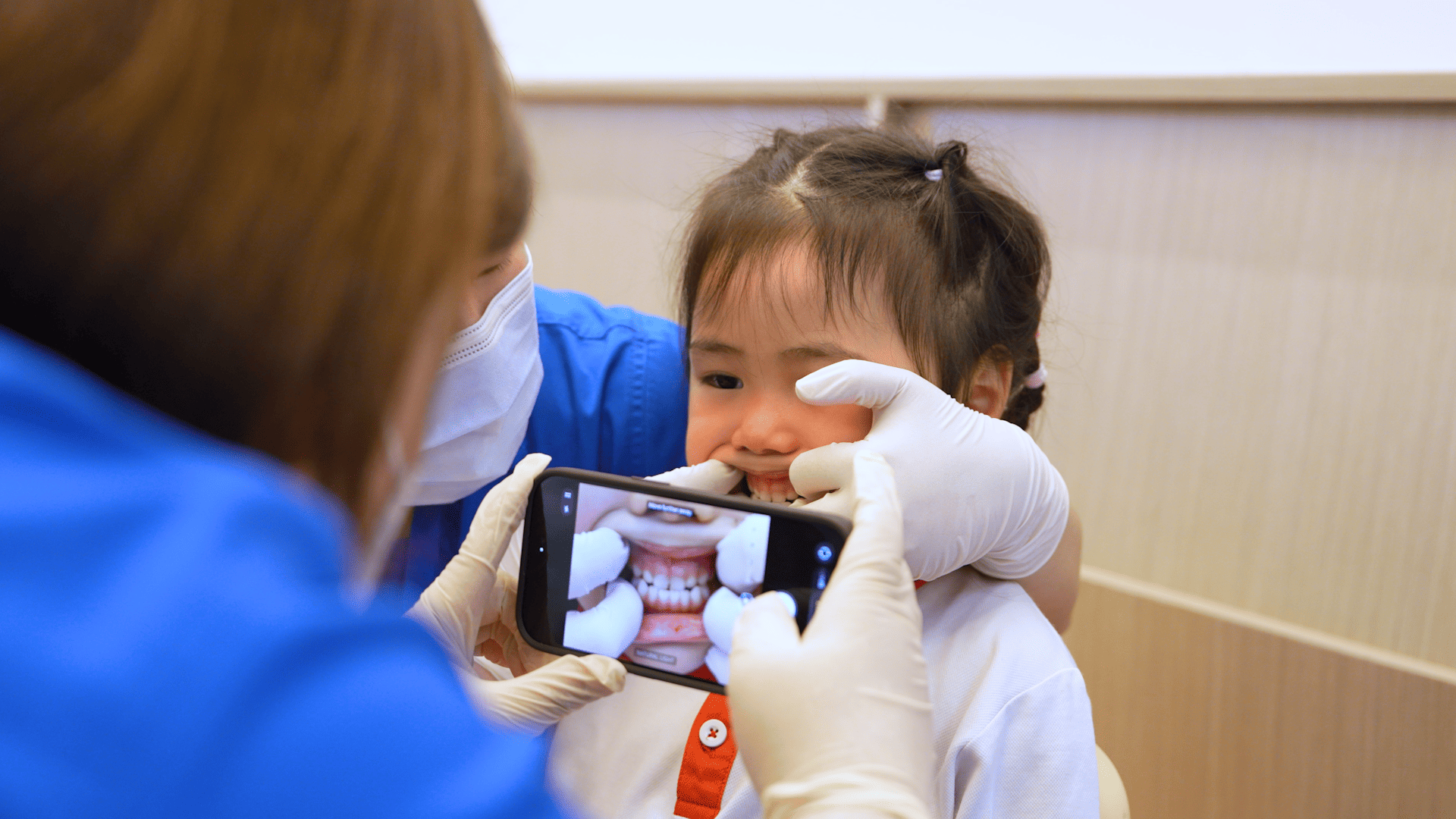
A HEADS-UPP team member captures intraoral images during preschool screening and dental assessment.
Thereafter, nurses capture five intraoral views of each child’s teeth during preschool screening sessions and upload them securely for review by a paediatric dentist.
A screening model built for earlier intervention
The paediatric dentist then reviews the images alongside the questionnaire, assessing visible plaque, gingival inflammation, enamel changes and caries, including behavioural risk factors. These results reflect more holistically on the assessment of each child’s dental risk and follow-up needs.
Mock-up demonstrating how intraoral images are captured and reviewed remotely.
For the assessment to be accurate, images captured must be consistent from the outset. Hence, training was coordinated for the HEADS-UPP health team staff on dental photo-taking, to better support reliable remote assessment.

Intraoral images captured allow paediatric dentists to assess oral health remotely.
Children are then triaged according to risk. Lower-risk children are directed to general dental care. Those at moderate to high risk without visible cavities are referred to the National University Polyclinics (NUP).
Finally, children who require more advanced intervention will be referred directly to the National University Centre for Oral Health, Singapore (NUCOHS) for specialist care.
Turning dental findings into clearer next steps
Ensuring families understand the assessment enhances the effectiveness of screening efforts. Personalised dental reports anchor the programme at that point of decision, translating assessment results into guidance that is easier for parents to understand and act on.
Each report includes annotated intraoral images, a caries risk classification and prioritised recommendations. The HEADS-UPP team will walk parents through the findings, reinforce preventive advice, and explain next steps, giving families a clearer route from detection to care.
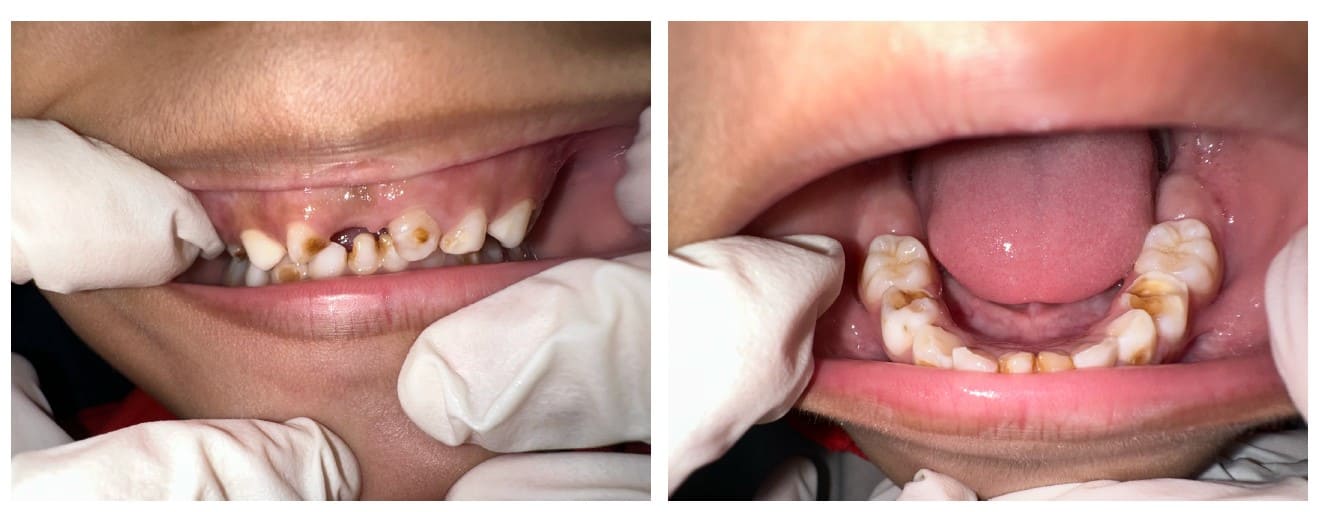
Intraoral images form part of the personalised reports shared with families to show visible areas of concern and for clearer follow-up.
Early findings suggest the approach is improving follow-through. As of 20 January, 355 children from 17 PCF Sparkletots preschools had gone through the programme, with most classified at moderate to high risk of dental caries.
Among children identified with caries, specialist follow-up attendance rose from the 13.3 per cent baseline in the previous screening programme to 57.5 per cent under the HEADS-UPP initiative, with more parents seeking care at general practitioner clinics and polyclinics.
A more structured route from screening to care
Follow-up findings also pointed to meaningful behavioural improvement, with the proportion of children classified at moderate to high caries risk falling from 93.3 per cent to 75.6 per cent after six to nine months. Parents also reported stronger toothbrushing routines, fewer risk-promoting habits and greater confidence in managing their child’s oral health.

The team explaining findings to children and caregivers, providing appropriate guidance and follow-up.
Lower-income children face the steepest oral health gap
HEADS-UPP also focused on children from lower-income families, where oral health inequity is already taking hold by the preschool years. Earlier research found fewer than half had ever visited a dentist, while follow-through after referral remained low. Disease burden also disproportionately affected these families, with 16 per cent of children accounting for 78 per cent of all caries lesions.
Why lower-income preschoolers remain a priority
Fewer than 50 per cent had ever visited a dentist
Only 13.3 per cent followed through after referral
Emergency service use and poorer oral health practices were more common in this group

Preschool-based screening reduced dependence on symptom-led visits and helped bring assessment closer to children who may otherwise be missed by conventional pathways.
Family accounts gave the findings a clearer human dimension. One caregiver described the report as systematic and easy to follow, while another said the programme imparted valuable lessons after their older children needed extractions and crowns, suggesting that clearer guidance can prompt earlier action.
Building the next phase of preventive dental care
HEADS-UPP points to paediatric oral health becoming more proactive, structured, and easier to scale. Apart from earlier detection, its longer-term value lies in how consistently that support can be extended to children who are most at risk.
The next phase looks toward incorporating artificial intelligence to support image review, questionnaire analysis and report generation. If developed well, that capability could help the programme reach more preschools and families with greater speed and consistency, while keeping clinical judgement at the centre of care.
In consultation with Adj A/Prof Chong Shang Chee, Head of Division and Senior Consultant, Division of Developmental and Behavioural Paediatrics, Khoo Teck Puat – National University Children’s Medical Institute, National University Hospital (NUH); A/Prof Catherine Hong Hsu Ling, Vice Dean (Research, Innovation and Enterprise), Faculty of Dentistry, National University of Singapore, and Senior Consultant, Division of Paediatric Dentistry, NUCOHS; and Dr Ishreen Kaur Dhillon, Academic Fellow, Faculty of Dentistry, National University of Singapore, and Associate Consultant, Division of Paediatric Dentistry, NUCOHS.